If you have not studied biology, it is likely that you only remember some of the basic notions you learned in school about this topic (like most people do…). But if you are pregnant, curious or you’re undergoing an assisted reproduction treatment, you may be a little more interested in it. In this article, Dr Monica Parriego, specialist in embryology and responsible for our Preimplantation Genetic Diagnosis Laboratory, offers us some data that you may not know or that could surprise you. Ready to level up?
- How is it generated and how big is an embryo initially?
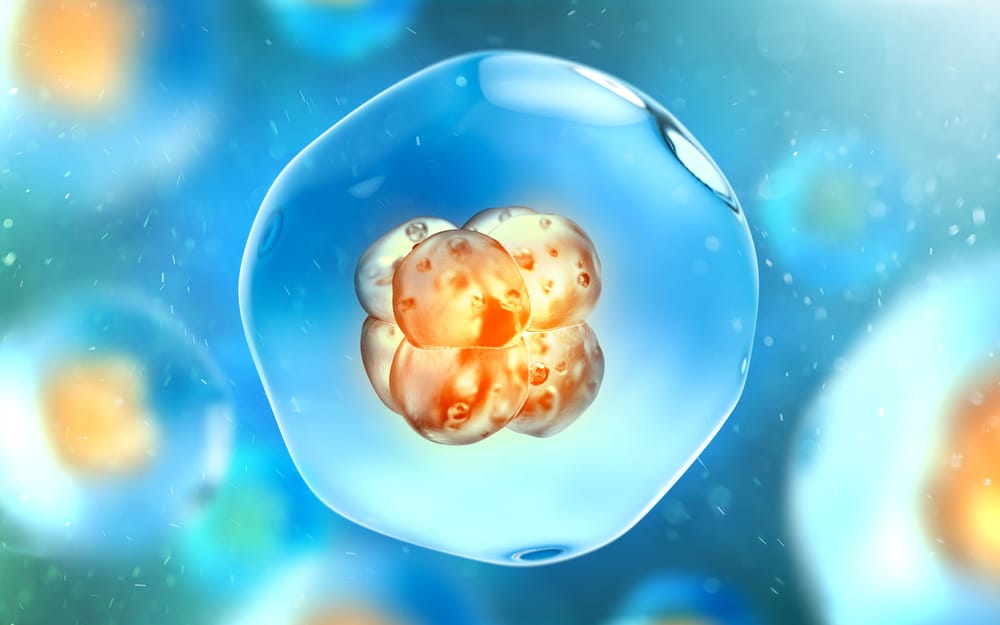
The human embryo is the result of the union of an egg with a sperm. That union results in its first cell, which is called the zygote. It is a spherical cell less than 1 mm in diameter surrounded by an envelope that will protect it until the moment of implantation. The zygote stage is short, it lasts approximately 25-28 hours, and from this moment cell divisions are produced continuously.
- How can we know if it evolves well or not?
On the first day of development, a properly fertilized ovule, or zygote, shows two nuclei, one with the genetic material of the ovule and the other with the sperm’s. Subsequently, these nuclei fuse and the embryonic division begins. An embryo with an optimal rate of development at two days of culture has 4 cells, and at 3 days, 8. From this point, the cells join together, and their count is no longer possible. At 5/6 days of culture, if all goes well, a complex structure composed of about 200 cells should be formed.
- How is a good quality embryo distinguished from another?
Although it seems very soon, the rhythm of division of the embryo in these first days, as well as the appearance of its cells, is already indicative of its quality. For this reason, it is essential to observe its evolution continuously during that stage. In addition to counting the number of cells, it should be noted if they have a similar size and a homogeneous appearance, and if the divisions have occurred at the correct times. All these parameters influence the ability of the subsequent development of the embryo and its implantation.
- Do you know what the time-lapse technology – incorporated in some incubators – is?
Embryos are very small structures not visible to the naked eye and the use of a high magnification microscope is required to observe them, although this involves removing them from the incubator and interrupting the optimal culture conditions. But the “time-lapse” incubators incorporate a camera that allows viewing the embryos from an external screen without having to remove them, which favours the stability of the process and makes it possible to obtain higher quality embryos. This technology consists of a sophisticated procedure for capturing images, by means of which videos are generated, from a series of photographs that are taken at certain time intervals (15-20 minutes). Thus, we can visualize the evolution of each embryo continuously, which allows a better assessment of its morphology and optimize its selection.
- Why do implantation failures occur?
There are several reasons why it can happen. In order for implantation to occur, a capable embryo, a receptive uterus and good communication between the two are required. Thus, any problem that affects any of the parties can compromise the establishment and evolution of pregnancy. In addition, there are other issues regulated by the laws of biology: sometimes the embryo, although its external appearance is good, is not progressing because the genetic information of its cells is not correct, or it suffers defects in the generation of energy. Likewise, anatomical problems of the uterus or alterations in the microbiota of this area can also make implantation difficult.
- How many embryos are usually obtained in an in vitro fertilization process?
The number of oocytes retrieved and embryos generated is very variable since it depends on multiple factors, maternal and paternal. There are different drugs that can be administered following different guidelines to obtain quality oocytes and sperm, although there are certain individual characteristics that we cannot modify (such as age). But what really influences the chances of pregnancy is the quality of the transferred embryo.
- What should I do if I want to donate my remaining embryos to other couples or be a recipient?
If your reproductive project has already been completed and you want to help other couples to fulfil their desire to be parents, the legislation in force in Spain allows donating the embryos of assisted reproduction treatments to other couples or women who need them. For this, the parents must sign an informed consent document, a donation contract, and their personal and family medical history to show that they have no history of any congenital disease. Moreover, some additional medical tests should be performed. In case you want to be an embryo recipient, you just need to request it. It is a good option when embryos cannot be generated with the ovules and / or sperm of the patients. In our centre we have an Egg and Embryo Donation Program that looks for the most appropriate option for each case.
- Is it true that in the first stage of development a human embryo is similar to that of a fish or that of a bird?
The theory was formulated by a German scientist named Ernst Haeckel in the mid-19th century and is still being studied at the University. This researcher had observed that early human embryos showed structures similar to those that appear in other animal species in adulthood, such as clefts reminiscent of gills or an extension of the spine that could lead to a tail. He called it a recapitulation theory, because he believed that during the early stages of embryonic development organisms “recapitulated” their initial evolutionary steps. Although the recapitulation theory has been partially rejected in its most literal version, some aspects of it remain accepted, such as the fact that the most primitive structures are formed in the early stages of development, and those acquired evolutionarily appear in later phases.